Eye drops are one of the most direct and effective ways to treat eye problems. Instead of a pill that has to travel through the entire body, a drop lands exactly where it is needed, working faster and with fewer systemic side effects in most cases. That directness is what makes them the first line of treatment for such a wide range of conditions, from something as routine as screen-related dryness to something as serious as glaucoma.
Most people have used some form of eye drop in their life, but not many know that the bottle on their bathroom shelf is doing something fundamentally different from the one at their doctor's office. Artificial tears and antibiotic drops share a format but nothing else. Understanding which type does what, and why, helps you use them correctly, avoid misuse, and know when to stop treating yourself at home and see a specialist.
1. Role of Eye Drops: Types, Uses & What Each Drop Really Does
2. Types of Eye Drops and Their Uses
2.3 Anti-Inflammatory Eye Drops
3. Warning Signs You Are Using the Wrong Eye Drop
4. Root Causes of Common Eye Issues
4.1 Tear Film Dysfunction (Root Cause of Dry Eye Syndrome)
4.2 Bacterial Entry into the Eye (Root Cause of Eye Infections)
4.3 Allergen Exposure (Root Cause of Allergic Eye Disease)
4.4 Increased Intraocular Pressure (Root Cause of Glaucoma)
5. How to Apply Eye Drops for Best Results
6. Prevention Tips to Help You Reduce Your Use of Eye Drops
7. Save Sight Centre's Expert Insights
8.1 Can I use artificial tears every day?
8.2 What is the difference between antibiotic and antiviral eye drops?
8.3 Do glaucoma eye drops improve vision?
The most common type, which is over the counter without a prescription, is artificial tears and lubricating drops. They are aimed at treating the dry eye syndrome that occurs when the eye lacks the production of tears or the production of tears is too rapid.
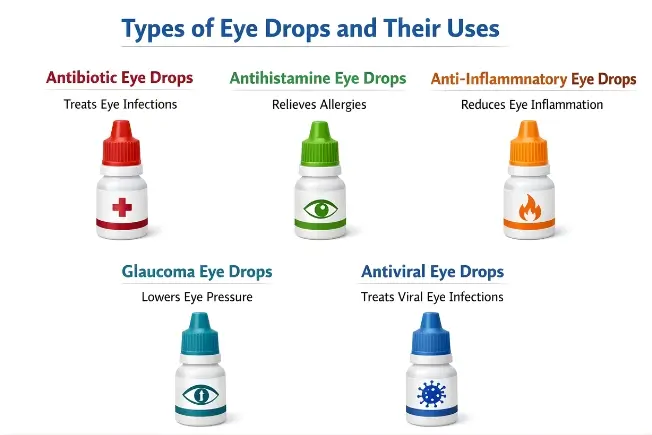
Antibiotic eye drops are used to treat bacterial infections of the eye, such as bacterial conjunctivitis, corneal ulcers, and contact lens-related infections. They work by killing the bacteria responsible for the infection. Commonly used antibiotic drops include ciprofloxacin, moxifloxacin, tobramycin, and ofloxacin, which belong to the fluoroquinolone or aminoglycoside groups.
Antihistamine eye drops are used to manage allergic reactions in the eyes, including those caused by seasonal hay fever, dust, or pet dander. When the eyes come into contact with allergens, histamine is released, leading to symptoms like irritation, redness, swelling, and watery discharge. These drops help block histamine and relieve discomfort.
Anti-inflammatory eye drops are broadly classified into corticosteroids and non-steroidal anti-inflammatory drugs (NSAIDs). Steroid drops such as prednisolone and dexamethasone are prescribed for inflammatory conditions like uveitis, keratitis, and post-surgical inflammation. They help reduce swelling, redness, and pain in the eye.
Glaucoma eye drops are the first line of treatment for managing increased intraocular pressure, the main cause of optic nerve damage in glaucoma. Unlike other eye drops, they do not improve vision or provide immediate noticeable relief. Their primary role is to prevent further damage and preserve existing vision.
Antiviral eye drops are used to treat viral eye infections, most commonly caused by the herpes simplex virus. These infections can affect the cornea and, if left untreated, may lead to scarring and permanent vision loss. Antiviral drops help control the infection and reduce the risk of complications.
Combination eye drops contain two active ingredients in a single bottle, usually an antibiotic and a steroid. They are used when there is both an infection and significant inflammation at the same time, such as after eye surgery or in more severe cases of conjunctivitis. For example, TobraDex combines tobramycin (an antibiotic) with dexamethasone (a steroid), while Zylet combines tobramycin with loteprednol. These drops help treat the infection while also reducing redness, swelling, and irritation.
Using the wrong eye drop does not help. In some instances, it actively postpones the right treatment or causes new problems. Some patterns are worth knowing.
If you are using artificial tears for an eye infection, the infection will only get worse, even if the immediate dryness appears to be a little better. Bacterial conjunctivitis requires antibiotic treatment instead of lubrication. Similarly, application of antibiotic drops for viral conjunctivitis, which has no greenish discharge and usually occurs in both eyes with a watery discharge, will not clear the infection and may contribute to antibiotic resistance.
Of all the drugs, steroid drops are perhaps the most dangerous to abuse. Using them for a viral infection, especially one caused by herpes simplex, may cause the virus to spread more aggressively in the eye, with potentially serious damage to the cornea. Anti-redness drops, which are used daily for weeks, are another trap.
The first step to knowing why you need a certain eye drop is to know what has gone wrong with the eye in the first place.
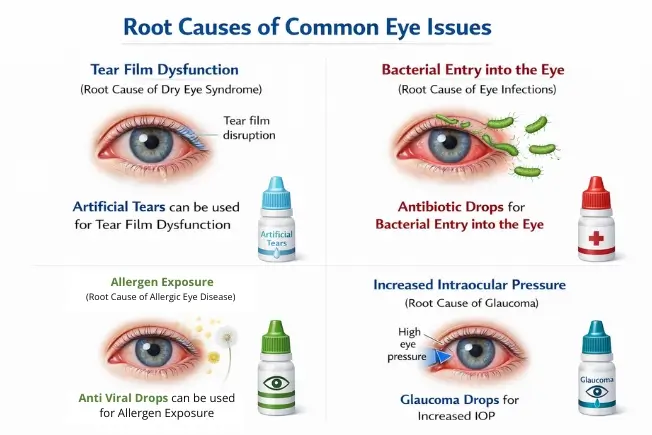
The tear film has three layers: mucus, watery, and oily, each playing a role in keeping the eyes lubricated. A problem in any of these layers can disrupt tear stability and lead to dry eyes. Reduced blinking, especially during prolonged screen use, further accelerates tear evaporation, making dryness worse.
Bacterial eye infections often begin when harmful microorganisms enter the eye. This can happen through touching the eyes with unclean hands, using contaminated contact lenses, or through the spread of infection from nearby areas like the sinuses or nasal passages.
Exposure to airborne allergens such as pollen, dust, or pet dander can trigger allergic reactions in the eyes. Individuals with a personal or family history of allergies are more prone to allergic conjunctivitis, with symptoms often worsening during high-pollen seasons like spring and autumn.
A rise in intraocular pressure is the primary underlying cause of glaucoma. This may occur due to genetic predisposition, aging, use of certain medications like steroids, or structural issues in the eye’s drainage system that prevent proper fluid outflow.
Even the right eye drop cannot work correctly if it is applied improperly. Many patients fail to reap the maximum advantage of their drug just because of the technique.
Wash your hands first before touching any eye drop bottle. Bend your head backwards, use one finger to push the lower eyelid downwards to form a small pocket, and with the other finger keep the dropper above the eye but not touching the eye or the eyelid. Put one drop in the pocket, close your eye, touch your finger, and press it on the inner corner of the eye for one to two minutes. This procedure, known as nasolacrimal occlusion, prevents the drop of draining into the tear duct and into the throat, which enhances absorption and minimizes systemic side effects, especially with glaucoma drops.
In case you are taking more than one kind of eye drop, you should wait a minimum of five minutes between them. Using them one on top of the other makes the latter drop to dissolve the former before it could do its job. When a patient with glaucoma is taking several drops, it is always preferable to set an alarm or have a small checklist to remain consistent because the effects of missed doses would accumulate over time.
Many conditions that necessitate eye drops can be minimized in frequency or severity by consistent daily habits.

Early detection means beginning drops when the pressure is only slightly raised, which requires fewer medications and less risk of side effects than beginning treatment late when there is already significant optic nerve damage.
Save Sight Centre ophthalmologists evaluate the eye condition of each patient before prescribing any eye drops, as the wrong eye drop prescribed for the wrong diagnosis can delay the recovery or cause complications. On-site diagnostic facilities enable the proper determination of whether an infection is bacterial or viral before thinking of using antibiotics.
Dry eye patients receive a comprehensive tear film evaluation, including meibomian gland evaluation, to determine if the cause of the dry eye is aqueous deficiency or evaporative dry eye before a lubricant is chosen. For patients on steroid drops for inflammatory diseases, regular checkups of pressure and slit-lamp examination are scheduled during the course of treatment. As part of the management of seasonal and chronic allergic eye disease, allergy patients in Delhi are also counselled about indoor air quality and pollution exposure reduction.
Yes, preservative-free artificial tears are safe to use as frequently as necessary throughout the day. If you are using preserved artificial tears, limit use to four times a day or less to avoid irritation from preservatives. If you are having to take drops very frequently, it is worth seeing an eye doctor.
Antibiotic drops are used for killing the bacteria and are used for bacterial conjunctivitis and corneal ulcers. Antiviral drops are aimed against viruses (in this case, herpes simplex virus infections of the cornea). Using antibiotic drops for a viral infection will not work.
No. Glaucoma drops are used to reduce the intraocular pressure so that more damage to the optic nerve can be prevented. They do not restore vision that has already been lost. This is why sometimes patients stop using them, thinking that they are not doing anything, when in fact the stability of their vision is itself the result of the drops working.
No. Corticosteroid eye drops are prescription only, as unsupervised long-term use can cause eye pressure to increase and cause cataracts. They should always be used under the supervision of an ophthalmologist with regular monitoring.
Most patients improve within two to three days of using antibiotic eye drops for bacterial conjunctivitis. The entire course should still be finished, usually in five to seven days, even if symptoms are getting better, to avoid re-infection and to reduce the chance of becoming resistant to antibiotics.
Copyright © 2025 | Save Sight Centre | All Rights Reserved.